NEW: Project ECHO’s 2023 Annual Report Read the Report
News & Stories
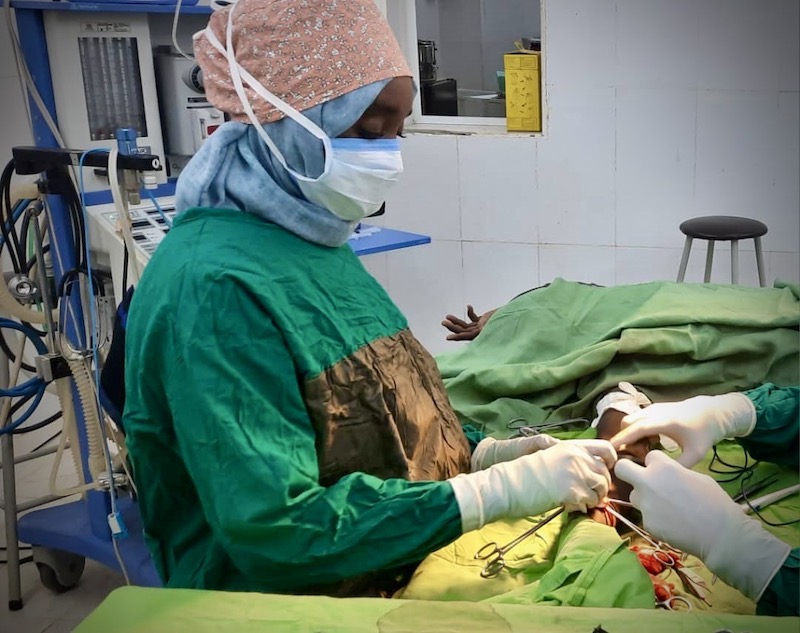
Emergency Preparedness
Project ECHO On the Frontlines with the Sudanese American Medical Association
Sudanese medical providers quickly learn critical war-time skills to save lives
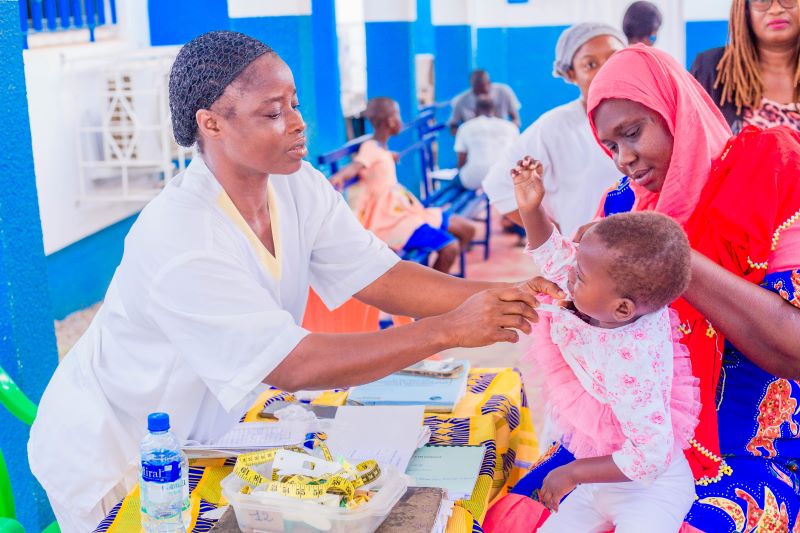
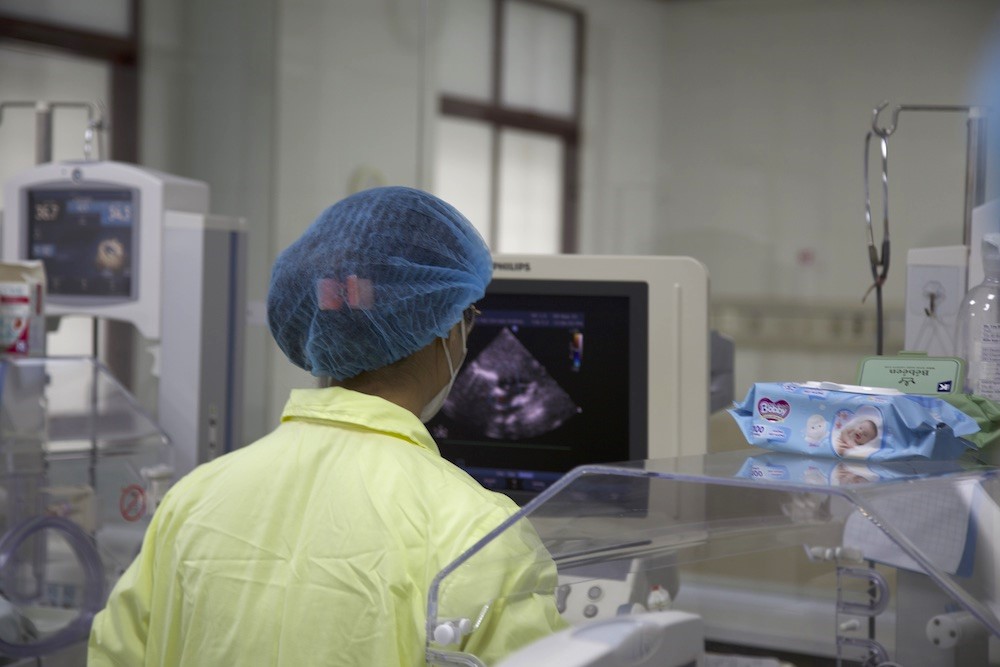
Maternal Child Health
‘Every Infant Matters’ for this Mother-Daughter Nonprofit Team
With the ECHO Model’s support, Dr. Shelly Batra and Dr. Radhika Batra reach more mothers around India with high-quality health care.
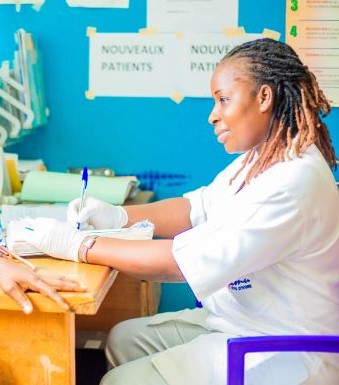
Health Care
ECHO Supports Infection Control Network in Africa
Project ECHO’s multi-year partnership with ICAN bolsters infection control throughout Africa.
563 Evidence-Based Impact
More than 500 peer-reviewed research papers have demonstrated the effectiveness of Project ECHO.
iECHO Platform
iECHO is our custom-built software platform. It supports our trusted human network of mentors and participants around the world.